Background:
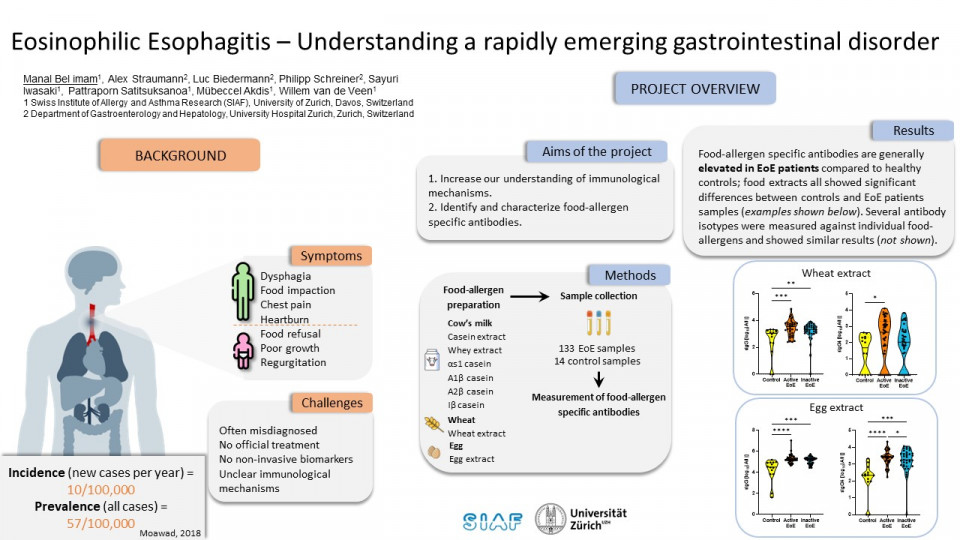
Eosinophilic esophagitis (EoE) is a chronic immune-mediated inflammatory condition that showed increased prevalence during the past decades. Although the mechanisms underlying EoE are not completely understood, several studies suggested the involvement of Th2 cytokines and antibody production. Also, food ingestion may play a role in EoE triggering, however it appears not to be a typical IgE-mediated food allergy. Rather, recent observations showed that EoE patients have high levels of IgG4 in esophageal biopsies and of circulating food antigen-specific IgG4. This preliminary analysis aimed to differentiate EoE patients according to the levels of food antigen-specific antibodies.
Methods:
Blood samples from 142 EoE patients were collected at the Swiss EoE Clinics at the University Hospital Zurich. The patients were categorized in active (>15 eos/hpf) and inactive (<15 eos/hpf) state of the disease, based on peak eosinophil counts in the esophagus. After processing blood samples, we used the plasma to measure food allergen-specific antibodies. Specifically, we measured total IgG and IgG4 against casein, whey, wheat and egg extracts, and the cow’s milk individual allergens alpha s1 casein, A1 beta casein, A2 beta casein and I beta casein by enzyme-linked immunosorbent assay (ELISA).
Results:
Among 142 samples, we could identify patients with highly positive, intermediate, and low levels of IgG and IgG4 antibodies specific for casein, whey, wheat, egg and cow’s milk individual allergens.
Summary and outlook:
This analysis will allow us to identify patients with high levels of food antigen-specific antibodies, which will be employed for a deeper analysis. In particular, we will isolate antigen-specific B cells and perform single-cell transcriptomics. Moreover, we will correlate this data with serum biomarkers identification, in order to ease the monitoring methodologies.